Extreme Heat & Physical Health
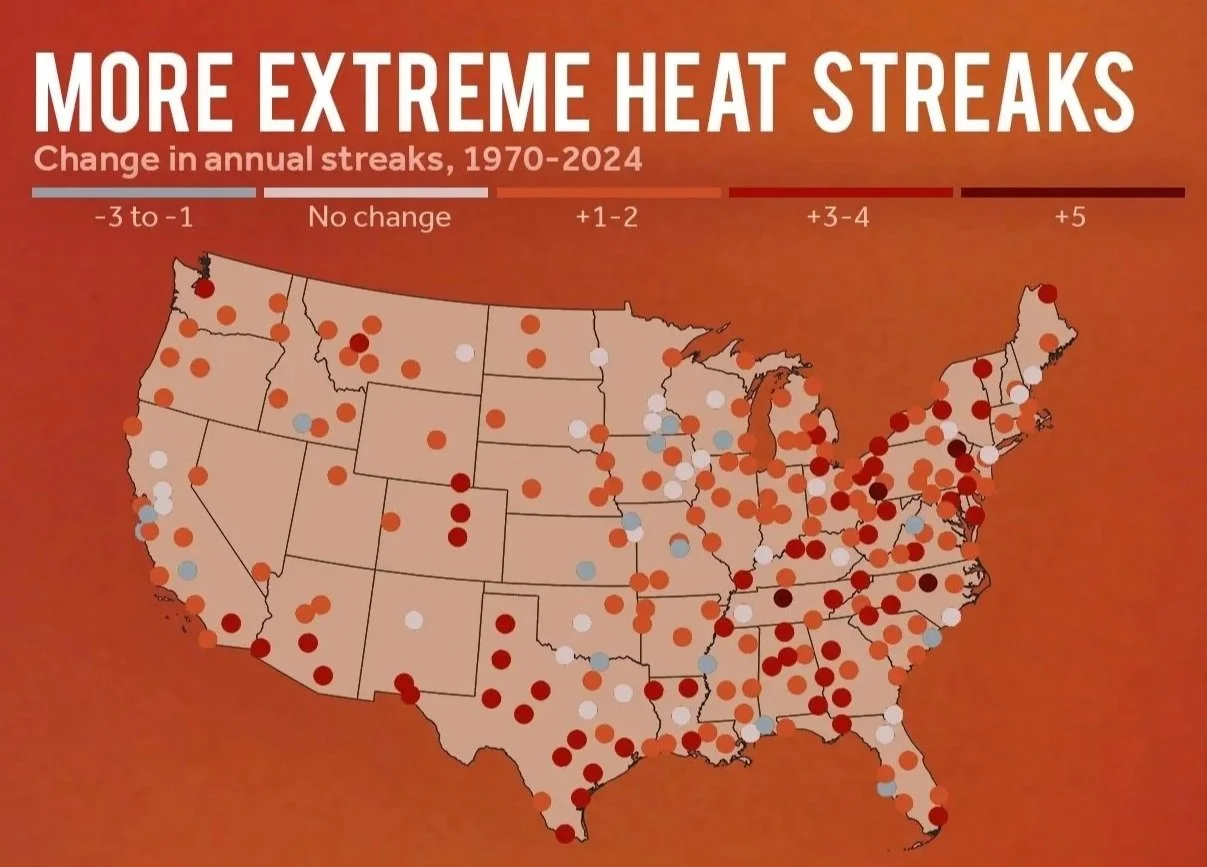
Extreme heat exposure is the leading cause of weather-related fatalities in the United States. Throughout the United States, we now see more frequent periods of extreme heat and humidity, a greater number of extremely hot days (defined as those in which the temperature is 95 degrees or higher), and more frequent and more widespread heat waves that begin earlier in the year and last longer than in the past.
Anyone who is exposed to extreme heat for prolonged periods can be at risk for heat-related illness or death, but there are certain factors that make some people more vulnerable than others, including health conditions, age, and socioeconomic status. Because most heat-related illnesses and deaths can be prevented, it is important to understand why the heat is so dangerous, who is most at risk, and what can be done to keep ourselves and others safe.
What Heat Does to the Body
Extreme heat can cause dehydration, heat exhaustion, and heat stroke, among other conditions. When the human body is exposed to heat, it must work harder to maintain a healthy, normal temperature. To cool down, there are two main mechanisms the body relies on: sweating and peripheral vasodilation, in which the blood vessels near the skin’s surface widen to help cool the skin. Both responses are regulated by the brain and require additional effort by the heart. The longer a person is exposed to extreme high temperatures, the more difficult it becomes for the body to keep up with the cooling demand, and this is when heat can turn deadly.
Dehydration
During extreme heat events, sweating can lead to dehydration, particularly if lost fluids are not regularly replenished. When a person becomes dehydrated, their heart must work harder to pump blood throughout the body. This additional effort increases cardiac demand and decreases heart function, potentially elevating the risk of heart attack.
Heat Exhaustion
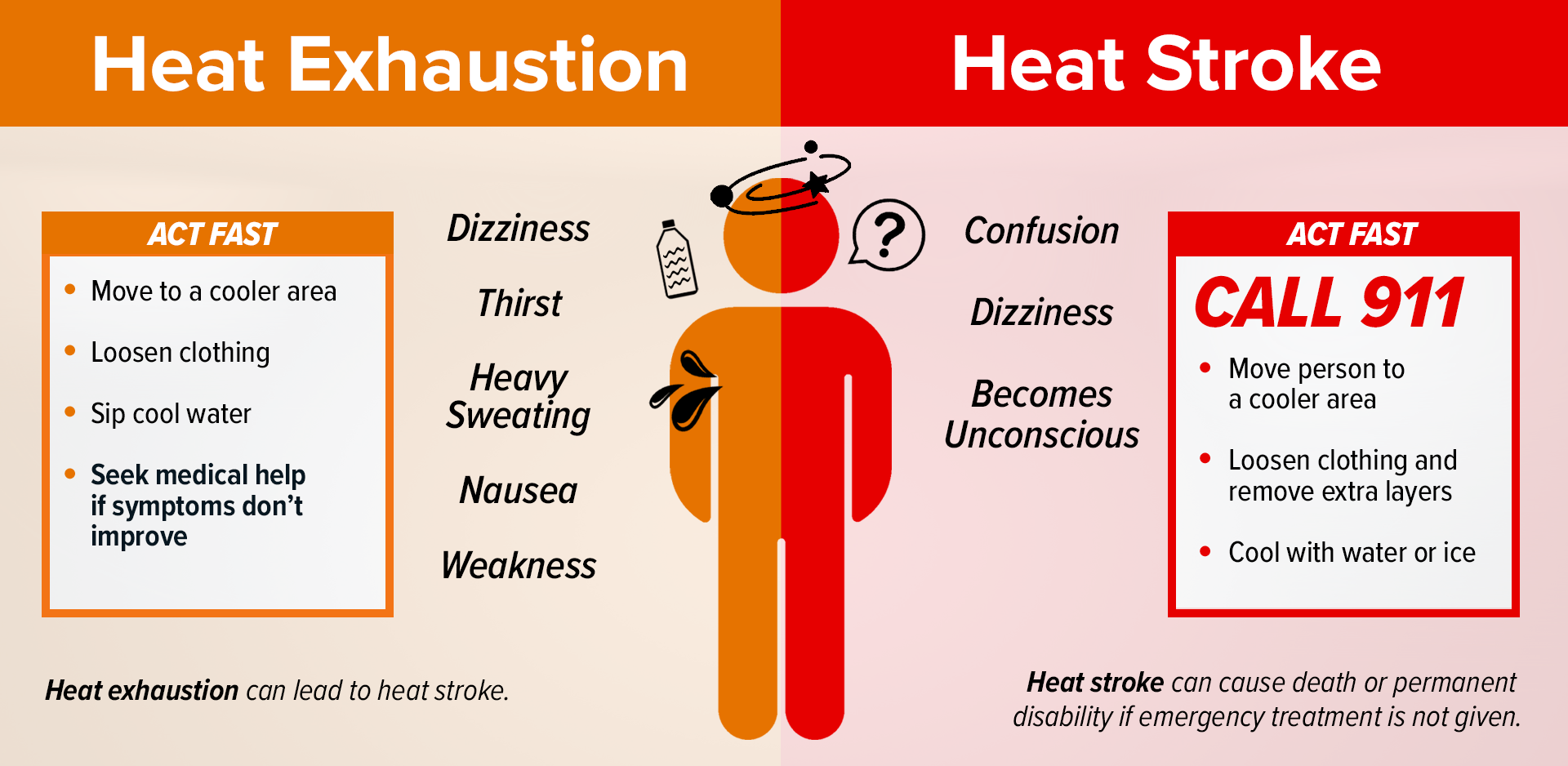
Heat exhaustion is typically less dangerous than heat stroke and can usually be treated without medical intervention. Some of the most common symptoms of heat exhaustion are heavy sweating, cool and clammy skin, headache, dizziness, fatigue, muscle cramps, and nausea or vomiting. If a person is experiencing heat exhaustion, their body temperature can typically be lowered by removing them from the heat, administering liquids, and cooling them with cold compresses or cold water.
However, heat exhaustion can quickly progress into heat stroke, which can be deadly without emergency medical assistance.
Heat Stroke
One of the ways in which the symptoms of heat stroke can be distinguished from the symptoms of heat exhaustion is by determining if the person is sweating. Unlike heat exhaustion, which causes profuse sweating, a person suffering from heat stroke will have minimal or no sweating. Their skin will appear red, hot, and dry as opposed to the “cool and clammy” skin of heat exhaustion. In addition, a person suffering from heat stroke will typically have a high body temperature, 104 degrees or more, and will often show signs of central nervous system dysfunction such as confusion, agitation, seizure, or loss of consciousness.
Heat stroke is a very serious condition that can be deadly without quick response and medical intervention. If a person is experiencing heat stroke, immediately contact 911 and move them to a cool and shaded area. To bring down their temperature, it will be necessary to try to cool the body as quickly as possible. Remove outer clothing, saturate remaining clothing with cool water, and cool the body directly by placing cold wet cloths or ice on the head, neck, armpits, and groin.
Heat & Chronic Health Conditions
Any person who is exposed to extreme heat for an extended period of time may be at risk for heat-related illnesses, but there are certain health conditions that increase this risk significantly and leave some people far more vulnerable to health complications than others due to the heat.
Cardiovascular Disease
According to the APHA, cardiovascular disease is the number one condition contributing to heat-related deaths during heat waves. Because extreme heat forces the heart to work extra hard to maintain a normal body temperature, this additional demand can be particularly taxing for a heart already weakened by cardiovascular disease.
One example of a cardiovascular disease is congestive heart failure, which causes fluid to accumulate in the legs and lungs and leads to reduced blood flow to other organs – both of which are exacerbated by extreme heat exposure. As a result, people with congestive heart failure face an increased risk of dehydration as fluids are retained in the body, an increased risk of organ damage as blood flow to organs slows, and an increased risk of heart attack as the heart struggles to pump the blood throughout the body.
Diabetes
Another condition that increases the health risks from extreme heat exposure is diabetes. Dehydration can happen more quickly for people with diabetes because high blood sugar causes more frequent urination. Diabetes may also affect a person’s ability to sweat or to dilate blood vessels in the skin, making it more difficult to cool the body naturally or to maintain a normal body temperature.
Heat & Medications
Ironically, the medications used to treat conditions like congestive heart failure can also increase the risk of negative health impacts from extreme heat exposure. Diuretics, which are used to treat heart failure by pulling excess fluid off the body, can worsen dehydration and can lead to electrolyte imbalances. And beta blockers, which are used to manage cardiovascular symptoms by relaxing blood vessels and slowing the heartbeat, can mute the cardiovascular response, making it more difficult for the body to cool itself through sweating and vasodilation.
The heat can also damage medications, making them ineffective or dangerous. Insulin, which is used to lower blood sugar in diabetics, must be kept cold or it can lose effectiveness or even raise blood sugar. And an asthma inhaler, a lifesaving device during an asthma attack, can explode if left in high temperatures for too long. Moreover, extreme heat can also increase the risk of adverse side effects from medications, such as an increased sensitivity to the sun (certain antibiotics) or a reduced ability to sweat in the heat (antihistamines).
Who is Most Vulnerable to the Heat
Clearly, there are certain health conditions and medications (or combinations of the two) that lead to increased vulnerability to heat-related illness or death. Congestive heart failure, kidney disease, diabetes, and cardiovascular disease are all significant risk factors for adverse health effects from extreme heat. Medications that treat these conditions can also raise the risk of illness or death from the heat, raising the vulnerability for this group of people.
Children, the elderly, and pregnant people are also at higher risk for heat-related illness or death. In children, factors such as smaller airways, less ability to cool their skin, more time spent outside, and a reliance on caregivers to keep them safe all raise the risk of heat-related illness. For the elderly, the risk increases not only because they are more likely to have some of the chronic conditions listed above, but also because they may live alone or lack access to resources that can keep them safe in high heat events. And pregnant women may be more vulnerable to heat health impacts due to pregnancy-related conditions and the medications used to treat them.
There are also socioeconomic factors that lead to an increased vulnerability to heat-related illness or death. Outdoor workers often spend hours in high temperatures without shade or water breaks. People living in cities have higher daytime and nighttime temperatures because of the urban heat island effect. Homeless people often have no safe way to escape the heat, leading not only to heat-related illnesses but also the risk of injuries, such as burns. And low-income people may lack air conditioning or be energy insecure, unable to afford to cool their homes.
Staying Safe in the Heat
The majority of heat-related illnesses and deaths can be prevented.
To stay safe in the heat it is important to:
· Limit outdoor activity
· Stay hydrated
· Take frequent rest breaks
· Avoid alcohol
· Seek out shade
· Take cool showers or baths
· Learn how to recognize and treat heat exhaustion and heat stroke
· Understand your risk factors
· Create a Heat Action Plan
· Listen to your body
Coming Up…
Hot temperatures tend to make people cranky, but heat’s impact on our mental health goes a whole lot deeper than that. In the next article from our Extreme Heat series, “Extreme Heat & Mental Health”, we will continue our investigation into the impact that high temperatures have on our health by looking at the role that heat plays in our mental health, including how mental illness and substance use disorder connect to heat-related illness risk and how certain psychiatric medications compound this risk.